Consumer Reports recently shared advice from audiologists and other experts about why it’s critical not to delay proper diagnosis and treatment when it comes to hearing loss. Below is an abbreviated version of the article which offers helpful insight into why people delay getting hearing aids and some of the health risks associated with postponing treatment.

Connie Vaughan, a 78-year-old retired office manager from Camden, Ark., didn’t think there was anything wrong with her hearing. Sure, she didn’t always understand what people were saying unless they were right in front of her. And yes, sometimes she did strain to hear her minister’s sermon on Sundays. But Vaughan told herself those people were mumbling.
Vaughan’s daughter, Lisa Christensen, an audiologist at Cook Children’s Medical Center in Fort Worth, Texas, and president of the American Academy of Audiology, suspected that her mother might have hearing loss. “Every time I visited, the TV would be blaring,” she says. “It was really difficult to speak to her on the phone. And she’d keep asking me to repeat things over and over again.”
Sensorineural hearing loss generally worsens over time. That’s because as we get older, the inner ear’s tiny hair cells, which convert sound waves into electrical signals that travel to the brain, may simply wear out. This can also occur after one-time exposure to loud sounds (such as an explosion), as a side effect of some medications (including certain chemotherapy drugs), or as a complication of conditions such as high blood pressure or type 2 diabetes.
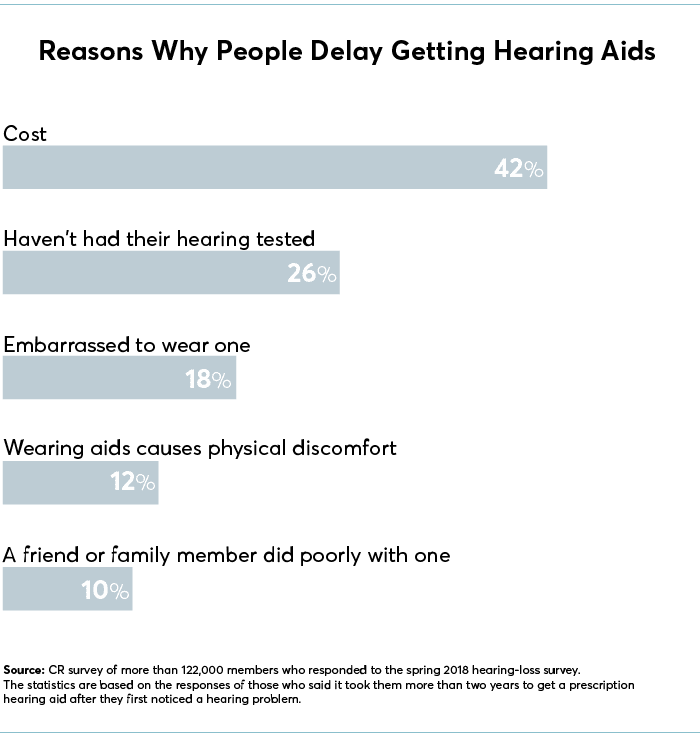
Why People Delay Treatment
Vaughan is just one of about 48 million people in the U.S. who have difficulty hearing. The number is expected to almost double by 2060, according to a study published in 2017 in the journal JAMA Otolaryngology-Head & Neck Surgery.
The biggest reason for this huge rise in hearing problems? Quite simply, the growing number of older adults. Another reason is the use of earbuds and headphones for listening to music, which may be leading to more hearing problems, especially among younger people, says James Denneny III, M.D., CEO and executive vice president of the American Academy of Otolaryngology-Head and Neck Surgery. They’re more likely to listen for long periods of time and may also be turning up the volume to overcome street noise.
Like Vaughan, many with hearing loss forgo treatment for years. Of the more than 122,000 CR members who responded to our spring 2018 survey on hearing loss, nearly one-third who acknowledged difficulty hearing had never had the problem diagnosed as such. And less than half of those with diagnosed hearing loss (or who thought they had the condition) had hearing aids.
One factor is that hearing loss, particularly the age-related type, often develops so slowly that it may go unnoticed. As Vaughan says, “the hearing loss came on so gradually, I just became used to it.”
Other people avoid getting help due to the stigma of hearing loss. A study in 2018 of 11 older adults with hearing loss, published in the American Journal of Audiology, found that participants felt ashamed and believed others saw them as “stupid.” And 18 percent of CR’s survey respondents who said they delayed getting hearing aids did so because of embarrassment.
“Looking back, I can see there were clear signs,” Vaughan says. “I guess I just didn’t want to admit that I really needed a hearing aid.”
Even after people are ready to seek help, the cost of aids—often thousands of dollars out of pocket—can put them off. There’s often little insurance coverage, if any, even from basic Medicare. In our survey, 63 percent of members said they waited at least two years after first noticing the problem to buy hearing aids, 42 percent of them because of the price.
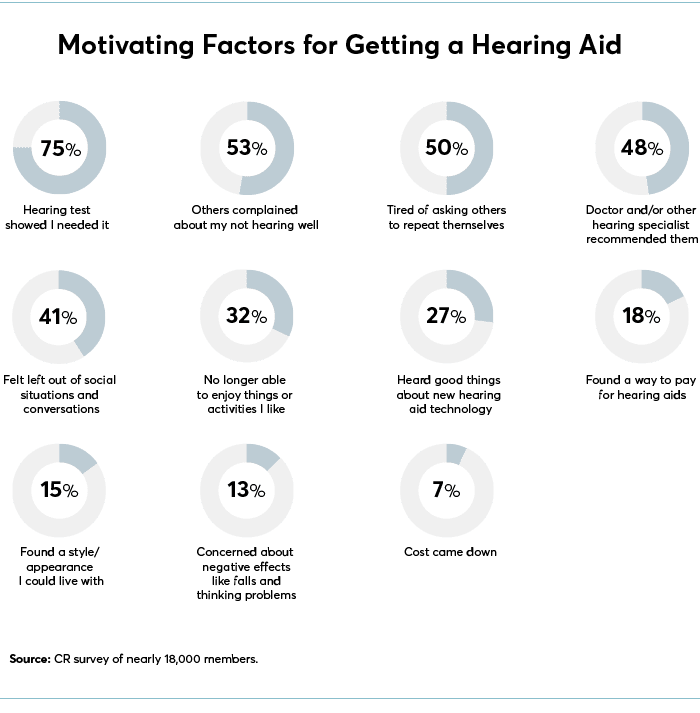
Health Risks of Hearing Loss
Those who acknowledge their hearing loss would do well to address it. A study published in 2018 in the journal JAMA Otolaryngology-Head & Neck Surgery found that among adults 50 and older, those with hearing loss were about 30 percent more likely to experience a fall. About 40 percent were more likely to be depressed, and about 50 percent were more likely to develop dementia over the 10-year study period.
One theory is that with hearing loss, the brain has to work harder to process sound, which may drain cognitive reserves faster, according to Maura Cosetti, M.D., director of the Cochlear Implant Center at the Ear Institute of the New York Eye and Ear Infirmary of Mount Sinai.
A life with untreated hearing loss can be one of loneliness and frustration. In fact, a 2017 review published in Trends in Hearing concluded that hearing problems take a significant toll on relationships.
Shari Eberts, 50, of New York City, knows this well. “There were so many social situations that I avoided, like going out to dinner or to a cocktail party, because I knew I would struggle the whole night to understand what people were saying,” recalls Eberts, a writer and hearing-loss advocate. “I would come home feeling absolutely exhausted. After a while, you figure, why bother? But then you end up isolating yourself even more.”
Both Eberts and Vaughan say their lives improved significantly when they began wearing hearing aids. Vaughan, for instance, is now able to fully participate in discussions in her Sunday school class and attend lectures without missing details. “Everything is so crisp, so clear,” she says. “I can have a conversation without constantly having to say, ‘What? What?’ ”
Experts concede that these pricey prescription devices can be challenging for people to use. “Unlike glasses, you can’t just turn them on and expect perfect, crystal clear hearing,” says Sarah Sydlowski, Au.D., Ph.D., audiology director of the hearing implant program at the Cleveland Clinic.
Nonetheless, the latest generation of aids can provide a significantly better experience than devices of the past—and they’re more discreet. What’s more, experts have extensive knowledge about how to protect and preserve hearing in the first place.
Use It or Lose It
Too many people, it seems, take their hearing for granted. In CR’s member survey, 30 percent of respondents said they had gone for more than 10 years without having their hearing checked or had never had a hearing test.
Although there are no national hearing screening guidelines for adults, you should have your hearing checked by an audiologist if you have concerns, and no later than age 50, says Sydlowski. Hearing evaluations are done by audiologists, who have a Ph.D. or a doctor of audiology (Au.D.) degree. (Some warehouse clubs have audiologists and hearing instrument specialists. The latter can check your hearing and help with aid selection and fittings, but they have less education and training.)
In the pure-tone test, which measures the ability to hear sounds at different frequencies, you wear earphones and raise your hand each time you hear a beep. In speech recognition testing, recorded words are played and you try to repeat them. This checks your ability to understand spoken words.
Depending on your test results and your risk factors for hearing loss—tinnitus, for instance, signals an increased likelihood of difficulty—the audiologist may recommend annual tests. If you’re found to have hearing loss, it’s important to take action as quickly as possible. “The longer you wait, the harder it will be to adapt to hearing devices when you do get them,” Sydlowski says. The reason: When the hearing nerve is understimulated by sound, it can begin to atrophy.
CR members speak out about important attributes of their hearing aids.
RECHARGEABLE BATTERIES
This allows you to charge aids every night and then wear them for a full 16 hours the next day, says Lisa Christensen, Au.D., president of the American Academy of Audiology.
SMARTPHONE COMPATIBILITY
You can stream music and calls from computers, smartphones—even TVs (with an additional accessory) through your aids.
TINNITUS MASKING
If you have chronic ringing in your ears, this offers soothing sounds to distract you.
AUTOMATIC NOISE ADJUSTMENT
Aids will automatically adjust to the noise level in the room, whether it’s soft, loud, or in between.
MULTIPLE PROGRAMS
They optimize your aid for different environments, such as a windy day or a party.
ADVANCED MICROPHONE FEATURES
They can help amplify the sounds you want to hear and minimize background noise.
Protecting Your Ears
Whether or not you have diagnosed hearing loss, it’s crucial to safeguard the hearing you have. Noise at or above 85 decibels (dB), which is considered moderately loud, like the noise of busy city traffic, may be harmful, depending on how long you’re around it. Anything between 85 and 100 dB, such as a lawn mower or motorcycle engine, can cause damage within an hour or two, and loud sporting events or rock concerts—which can clock in around 110 dB—can damage ears within 15 minutes.
If you know you’ll be around noise that’s at or above 85 decibels, especially on a recurring basis, use comfortable, well-fitting earplugs or earmuffs designed to bring your exposure down to safe levels, suggests Vickie Tuten, Au.D., an audiologist and a coordinator for the American Speech-Language- Hearing Association’s Special Interest Group 8: Audiology and Public Health. You can check product labels for noise reduction ratings. (For more, see CR’s series on noise in consumer products.)
Only 8 percent of adults in the U.S. say they regularly wear earplugs or protective headphones at loud athletic and entertainment events, according to the Centers for Disease Control and Prevention. But this simple step can make a big difference. A 2016 Danish study in JAMA Otolaryngology-Head & Neck Surgery found that people who wore earplugs for a 4½-hour outdoor concert were much less likely to experience temporary hearing loss—a sign of possible permanent damage—than those who went without.
When listening to music on devices such as a smartphone, consider noise-canceling headphones (see “Hearing Helpers for Music, Phone Calls & TV”). Keep music at no more than 60 percent of maximum volume for no more than an hour a day.
And last, follow a healthy lifestyle. Research suggests that smoking may increase the risk of hearing loss. But a healthy diet may reduce it. A 2018 study in the Journal of Nutrition found that women who followed eating plans like a Mediterranean-style diet or the DASH diet (both rich in produce and whole grains) had about a 30 percent lower risk of moderate to severe hearing loss.
Advances in Technology
Only 20 percent of people who could benefit from hearing aids wear them, according to the National Institutes of Health. That’s due to a variety of reasons—including, for some, the assumption that they won’t help enough.
Lisa Fried, 45, of New York City, gave up on her first set of hearing aids after several months. “They were useless for filtering out background noise,” she says, “so I felt like in many social situations, like a crowded restaurant, they made it harder to hear, not easier.”
When Fried tried again two years ago, she was pleasantly surprised. Aids have now become sleeker, smaller, and more able to minimize feedback and distracting background sounds, once common annoyances. Fried’s new Oticon Opn 1 aids screen out almost all of “that awful feedback and background noise,” she says.
Her aids are also Bluetooth-enabled, allowing her to take phone calls and listen to podcasts right through them. Some aids come with even higher-tech tools, such as sensors to detect your heart rate or the ability to send alerts to emergency contacts if you fall.
Those features may be useful for select users, but even modest devices may now offer enough benefits for most people. “There’s often a belief that if you have a hearing aid with fancy features and all the bells and whistles, it will result in a better outcome, even though there’s evidence to suggest that’s not the case,” Sydlowski says. In fact, a study published in 2016 in the journal Ear and Hearing found that people with premium models reported no more satisfaction or quality of life improvement than those whose aids had fewer special features.
Making the Most of Your Aids
When you first get your hearing aids, the audiologist should adjust them to match your needs; make sure they fit you comfortably; explain how to use, clean, and store them; show you how to change the batteries; and counsel you on the sounds you can expect to hear.
At home, wear your aids as much as comfort allows to help you get used to the feel of the devices and sounds that have gone unheard for years. “Put them on (early in the day) and try to leave them on until you go to bed at night,” says Deborah Culbertson, Ph.D., CCC-A, an audiologist and clinical professor at East Carolina University’s department of communication sciences and disorders.
To make sure your aids are properly programmed, return to your audiologist after the first two weeks for tweaks. You may need additional adjustments from time to time.
And last, be realistic about what hearing aids can do. They can help you hear better in certain situations, but they won’t return your hearing to normal. “People always ask, ‘What can restore my hearing?’ and the answer is, there’s nothing that can reverse nerve damage,” says Elizabeth Levine-Davis, Au.D., an audiologist at the New York Eye and Ear Infirmary at Mount Sinai. “It’s not like putting on a pair of glasses and suddenly experiencing 20/20 vision. Even so, today’s hearing aids are much more sophisticated than they ever were, and do a pretty good job at satisfying patients even in the most difficult situations.”
Source: Consumer Reports





